Cardiovascular image and data management: A technical and clinical evolution

Some of you remember the old days – the smell of dark room chemicals, quiet of massive film libraries, and presence of office managers surrounded by towering stacks of film jackets. The Cardiovascular Picture Archive and Communication Systems (CPACS) revolutionized images and workflows, enabling software to help cardiology store and access appropriate files. They also set the industry on a path that would lead to Cardiovascular Information Systems (CVIS).
It all started when Cardiology had to address several challenges to decommission film and video and move into the digital world of CPACS. While the image workflow was transforming, there were still significant amounts of paper to deal with, such as echo studies and measurements, stress lab results, EKG interpretations. The workflow was still largely paper oriented.
In the late ‘90s, movements toward registries and quality improvement helped cardiology make the transition to CPACS. A few years later, when the Centers for Medicare and Medicaid Services (CMS) introduced penalties for certain readmission rates, four of the six targets were cardiovascular.
These quality and regulatory requirements mandated more structured reporting from the cardiovascular service line, which meant moving an incredible amount of data back and forth between healthcare payers and healthcare providers. In this environment, CPACS became central to every cardiology department.
CPACS are just one component of CVIS
But cardiology soon realized it needed more than just a place to archive data; it needed a robust infrastructure that can bring in data and have it flow through the service line. It needed to evolve from a CPACS to a CVIS.
A true CVIS has wide-ranging benefits for people in different roles across the service line. Cardiovascular clinicians, for example, have simple and quick access to prior and related studies. They can easily review historical information to build a narrative in the clinician report. Department managers have access to productivity reporting, which is helpful for accreditation processes. Clinical managers have even richer support for clinical data registries, but can also use it to create case reports, clinical reports and support research. Executive leadership can use an CVIS to look from the department level through multiple facilities to evaluate productivity.
4 steps to advance from CPACS to CVIS
If an orgnization just has a CPACS, there are some fundamental questions to ask that can help them advance on their journey to a CVIS. Let's look at the steps within an example of a team that wants to improve service for patients with heart failure:
Step 1: What data do you have?
To focus on patients with heart failure, an organization might start with the electronic health record. Is the admission diagnosis accurate? Is this the best source of this information, or should it come from the heart failure clinic or echo lab instead?
Step 2: What data could you have?
Next, teams should assess all the data that is available to them. What is the output from the echo lab, based on the current workflow? If you had additional information, such as the time it takes from a patient receiving an order to being on the treadmill? What more could you do with it?
Step 3: How can we optimize the workflow?
Organizations need to understand the capabilities of their vendors and determine which workflows can bring the most benefit to their organizations. In this case, the organization could evaluate the data going into the lab and determine how automating it might help them improve accuracy or avoid duplication.
Step 4: What other benefits can we get from better, faster access to data?
One way for clinicians to get a handle on increasing amounts of data is through structured reporting, which has been implemented in many cardiology departments today. Consistent, complete, accurate data documentation in structured reporting supports clear and consistent care communication and provides a resource for evaluating and improving outcomes.
Every department has its own challenges and ways that their role in patient care interacts with other departments. For example, a change in post-procedure/pre-discharge echo documentation may reduce length of stay and could improve patient satisfaction.
In my experience, pulling together a data infrastructure for an effective CVIS is not simply assessing features and functionality of the technology. Rather, it’s asking the right questions about what the organization is trying to accomplish to improve the patient and clinician experience.
Related Articles
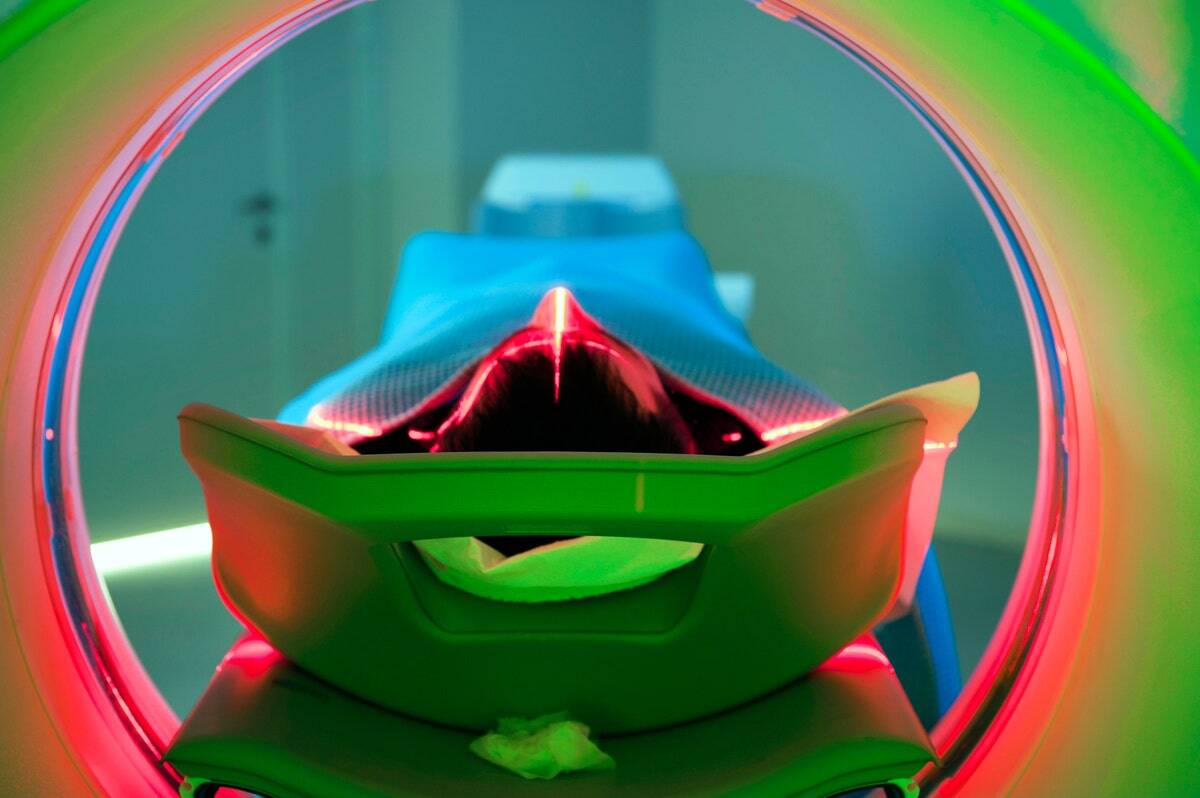
The 4 imaging AI questions we all need to be asking
By David Gruen | 6 min. read
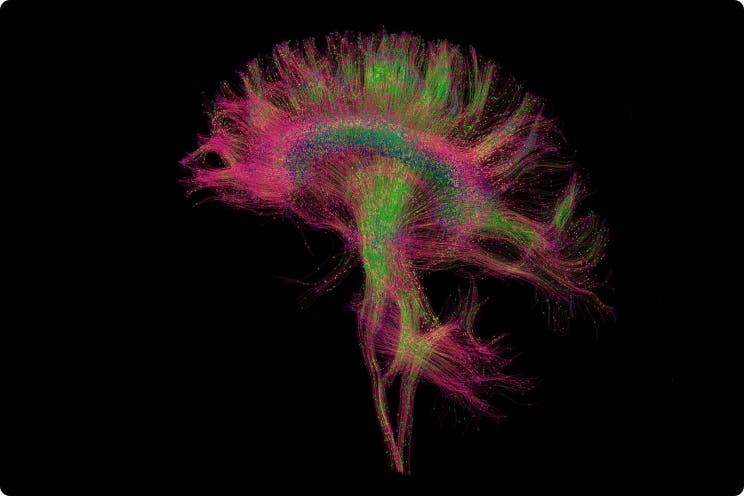
4 Ways this RSNA Panel Laid Out The Future Of Imaging AI
The paths forward to more rapid and widespread AI adoption in medical imaging.
By David Gruen | 6 min. read

Beyond KLAS rankings: building client relationships at Merative
By David Gruen | 3 min. read
Ready for a consultation?
Our team is ready to answer your questions. Let's make smarter health ecosystems, together.
